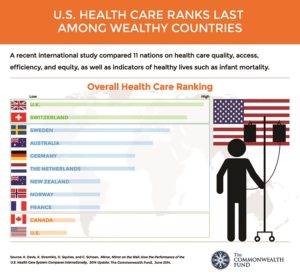
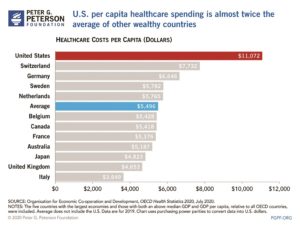
What if you don’t have Covid — but you still need a doctor?
This question became more urgent in 2021, when many people moved to the Outer Cape to escape the cities, but few of them were home health aides, nurses, or doctors. There is a critical shortage of all of them right now.
The workers who keep the elderly out of nursing homes are mostly women. Home health work is “not highly valued or well paid,” Geovana Pinheiro, a certified nursing assistant, said in October.
Most clients pay private home care agencies $30 to $35 per hour; but the caregiver takes home only half of that. Working 40 hours to bring home $400 a week after taxes isn’t practical on Cape Cod, Pinheiro said. Some of her colleagues have left the field to take higher paying positions where they can earn $17.50 an hour — like at Stop & Shop.
Meanwhile, patients of all ages are having a hard time getting a doctor. Outer Cape Health Services, the only provider on the Outer Cape, is inundated by a combination of new people moving to the area and retiring mid-Cape doctors whose entire panel of patients — hundreds at a time — are showing up at OCHS’s door.
New patients have to wait six months to see a doctor, CEO Patricia Nadle told us in November.
Weak systems become weaker when tested. The pandemic has further challenged a struggling mental health and addiction treatment system. In September, I interviewed Kim Powers, a longtime harm reduction specialist, who was fired from the AIDS Support Group of Cape Cod. She said she and the agency had significant disagreements over how to do keep drug users as safe as possible. ASGCC declined to comment.
Powers now drives around with clean needles, first-aid kits, fentanyl test strips, and other supplies to meet drug addicts where they are, which is often alone in their homes or in homeless camps. Isolation and fentanyl are a deadly combination.
Through Sept. 2021, the state Dept. of Public Health recorded 1,613 opioid overdose deaths (confirmed and estimated). That is 21 more deaths than in the first nine months of 2020, which had registered a 5-percent overdose death increase from the same period in 2019.
Opioid addiction became an epidemic because of the fraudulent marketing and overprescribing of painkillers such as oxycodone beginning in 1995. Drug companies and distributors have been sued, and Massachusetts is poised to receive hundreds of millions of dollars from litigation settlements with Big Pharma.
The money may bring a sea change to addiction treatment.
“We will be looking at people like Kim Powers to help us think it through” and find new ways to attack the problem, said Dr. Alexander Wally of Boston Medical Center.
With so much death of late, it is hard to find a silver lining. But maybe pulling death away from the health-care business offers a ray of light.
Since 2015, Dawn Walsh has been leading death cafés and advocating for green burials. In 2019, she founded the Lily House, a nonmedical, volunteer-run nonprofit where residents can die in a hospice house with 24-hour care but without the institutional coldness of a nursing home. Walsh formed a board of directors and obtained nonprofit status but did not have a house. That is, until she met Sandra Wonders.
Wonders, of Wellfleet, spent 25 years after retirement from the state Dept. of Developmental Services as an ombudsman at nursing homes, and she knew she did not want to die in one. Before Wonders died at home on March 11 of brain cancer, she donated her four-bedroom house to become the first Lily House.
Wonders “felt an obligation to give to other people what she was able to experience,” said her niece, Michelle Ouellette. “She was the definition of the word ‘altruistic.’ ”